658a5b2dc3c37bfbee9a8e29ebd1c516.ppt
- Количество слайдов: 90

การใชยาลดระดบนำตาลในเล อดอยางสมเหตผล ในกลมผปวยเบาหวาน ภญ. สพชชา อยสข เภสชกรชำนาญการ โรงพยาบาลสรนทร
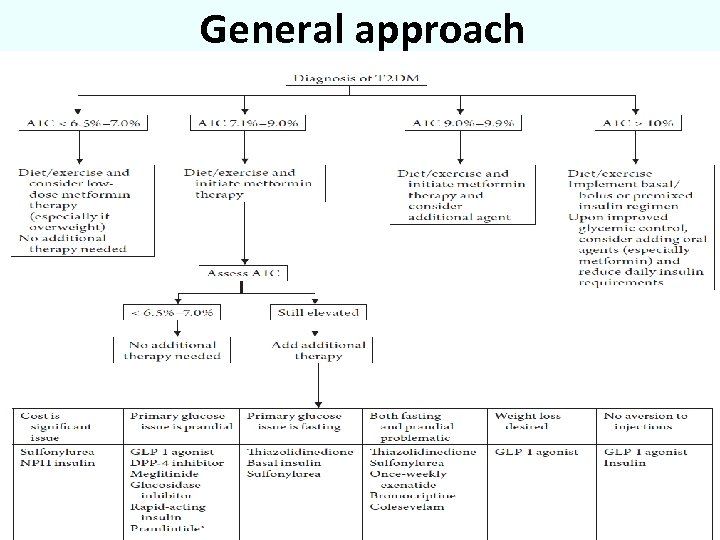
General approach 2
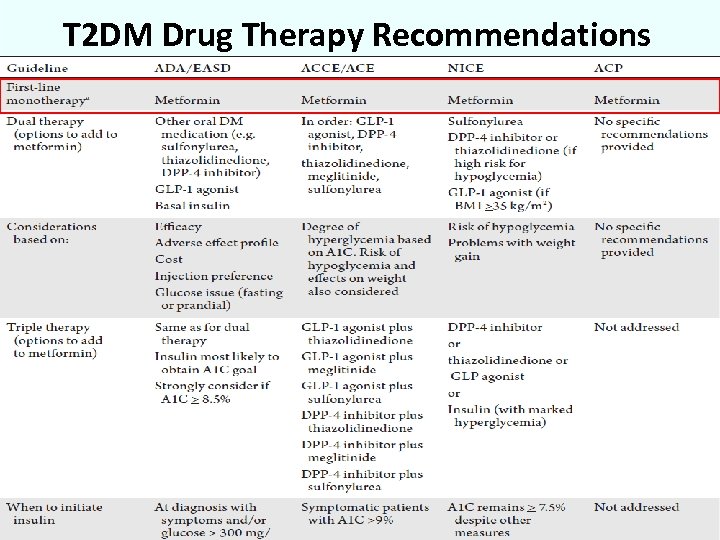
T 2 DM Drug Therapy Recommendations 3

ยาลดระดบนำตาลในเลอด (Antihyperglycemic Drug) • • Sulfonylurea ---glipizide, glibenclamide Rapid acting insulin secretagogue--repaglitanide Biguanides --metformin Thiazolidinediones----Pioglitazone (Actos) Alpha-glucosidase inhibitor---Acarbose DPP-4 inhibitors---sitagliptin (Januvia) SGLT 2 inhibitors---Canagliptin Insulin
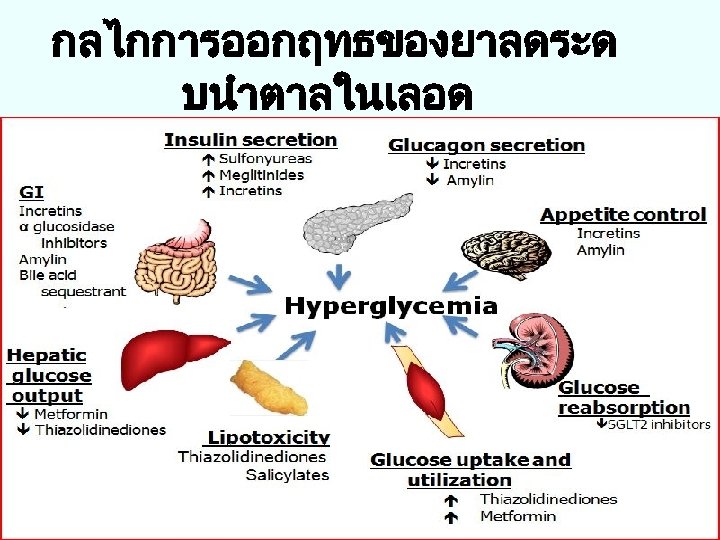
กลไกการออกฤทธของยาลดระด บนำตาลในเลอด
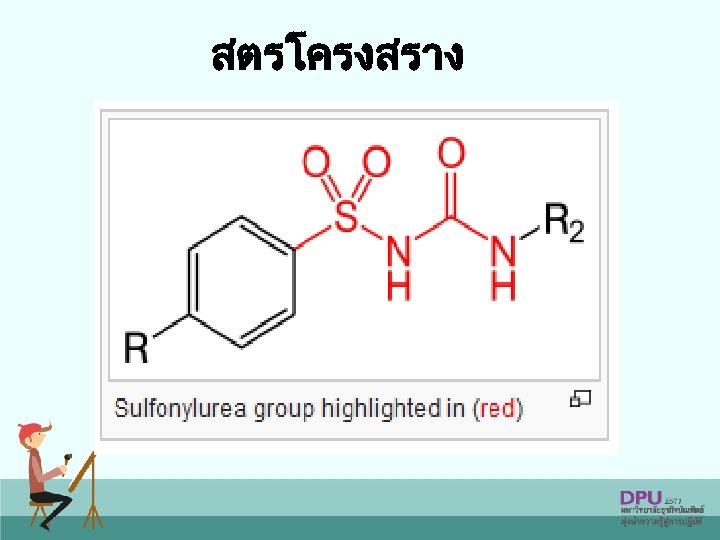
สตรโครงสราง
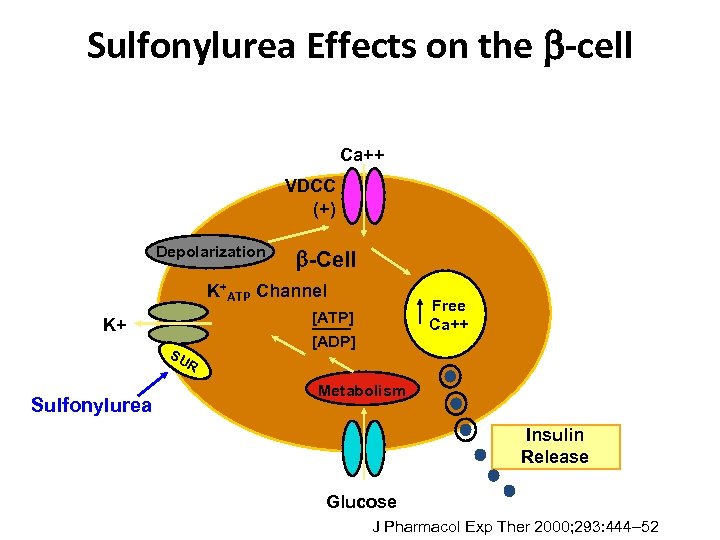
Sulfonylurea Effects on the -cell Ca++ VDCC (+) Depolarization -Cell K+ATP Channel K+ SU R Sulfonylurea Free Ca++ [ATP] [ADP] Metabolism Insulin Release Glucose J Pharmacol Exp Ther 2000; 293: 444– 52

Sulfonylureas • Hemoglobin A 1 C lowering of 1%– 2% • Decreases FPG ~ 50 - 70 mg/dl (minimal decrease in postprandial) • The higher the baseline Hb. A 1 C the greater the effect • Fifty percent of maximal dose begets 80% of drug efficacy • A 5%– 10% primary failure rate; 5%– 10%/year secondary failure rate 8
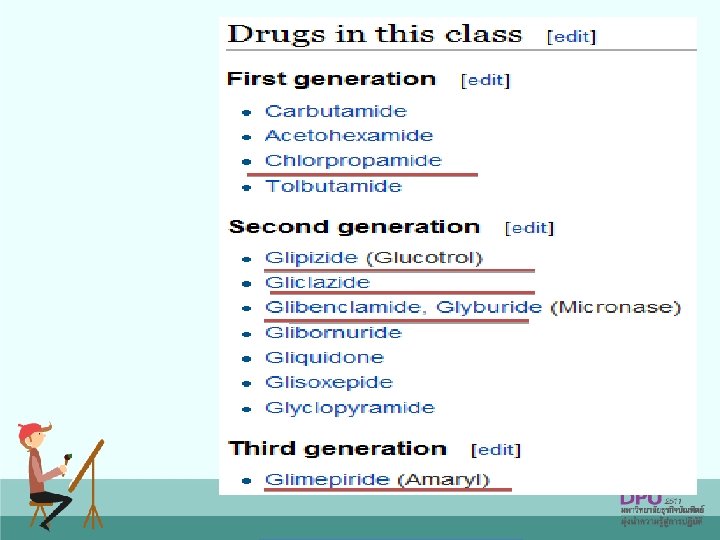
Comparison Drugs Initial dose Dosage range(mg/day) Elimination (M=hepatic metabolism R=Renal) Glibenclamide, Glyburide (Daonil) 2. 5– 5. 0 mg once or twice daily 2. 5– 20 50%M, R Gliclazide (Diamicron) 80 mg once or twice daily 40 -320 (30 -120 for MR) M, 80%R Glipizide (Minidiab) 5 mg once or twice daily 2. 5– 20 90% M, R Glimepiride (Amaryl) 1– 2 mg once daily 1– 8 40% M, 60%R Gliquidone (Glurinor) 15 mg once daily 15 -120 95% M, 5%R

Sulfonylureas Adverse effects: • Hypoglycemia • Weight gain • Less common: Rash, photosensitivity, dyspepsia, nausea/vomiting, headache Contraindications: • Hypersensitivity to sulfonamides • Diabetic ketoacidosis • Type 1 DM • Severe liver or kidney disease • Hypoglycemic unawareness (Beware for NPO) 11

ADR Weight gain Hypoglycemia Headache ไมควรใช glibenclamide ในผปวยทมการทำงานของไตบกพรอง (Scr > 1. 5 mg/dl หรอม GFR < 30 ml/min/1. 73 m 2) • ระวงในผปวยทมประวตแพยา sulfa • •

Rapid acting non-sulfonylurea insulin secretagogue

Meglitinides • Very similar to that of sulfonylureas in increasing insulin secretion from the pancreas but with a more rapid onset and shorter duration of activity • Glucose-dependent activity • A 1 C reduction: Repaglinide 1. 6%, Nateglinide 0. 8%, Mitiglinide 1. 3% • Most effective on postprandial glucose excursions • Metabolize by CYP 2 C 8, 3 A 4 14

Meglitinides • Mitiglinide(Glufast) – Initial: 5 mg 3 times daily with meals – Maximum dose : 20 mg 3 times daily • Repaglinide(Novonorm) – Initial: 0. 5– 1 mg 15 minutes before meals – Maximal daily dose: 16 mg • Nateglinide(Starlix) – 60 -120 mg 15 minutes before meals – 60 mg if A 1 C near goal • Can be increased in weekly intervals if needed • If skip a meal, skip medication 15

Meglitinides • Adverse effects: Hypoglycemia (though less than with sulfonylureas), weight gain, upper respiratory infection • Contraindications/precautions – DM type 1, DKA – Hypoglycemia unawareness – Caution in concomitant use of repaglinide and gemfibrozil, can lead to greatly increased repaglinide levels 16
Biguanide
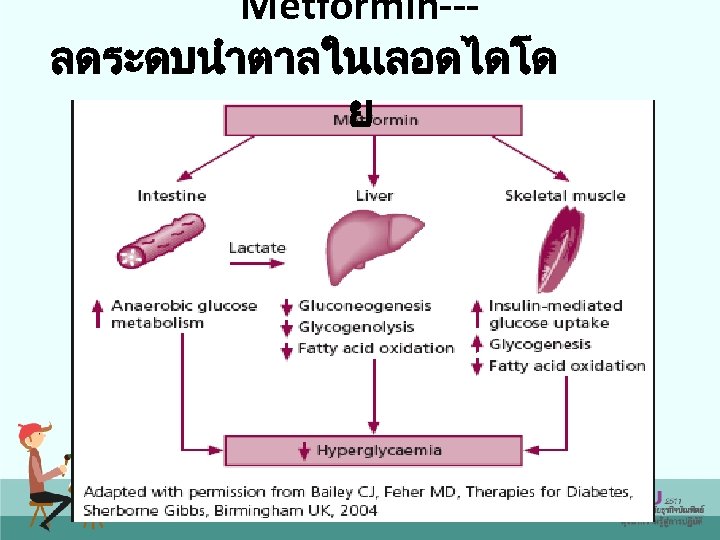
Metformin--ลดระดบนำตาลในเลอดไดโด ย

The Biguanide Effect • Inhibit oxidative metabolism – Increases NADH – Suppresses gluconeogenesis – Decreases the GI absorption of glucose • Intracellular redox potential shifts from aerobic to anaerobic metabolism • Decrease in pyruvate carboxylase activity (rate limiting enzyme in the formation of glucose from lactate) results in decreased hepatic metabolism of lactate • Symptoms: acidosis, nausea, vomiting, increased respiratory rate, abdominal pain, shock, and tachycardia

Metformin • Primarily inhibits hepatic glucose production • Secondarily some improvement of peripheral insulin resistance • May decrease intestinal absorption of glucose (small intestine) • Hemoglobin A 1 C lowering of 1%– 2% • Primarily reduces FBG(~ 50 - 70 mg/dl) • 5%– 10% per year secondary failure rate 20

Metformin Improved CV outcomes No hypoglycemia as monotherapy Positive lipid effects 500 mg once or twice daily with food to start (decrease GI adverse effects) • May take 2 -4 weeks to see maximum benefit • Maximal dose: 2550 mg/day • Common dose: 1 g 2 times/day • • 21

The Cardiovascular Effects of Metformin

metformin • In meta-analysis, metformin in Type 1 DM ; – reduce insulin requirements (6. 6/day, P< 0. 001), – small reductions in weight – Small totol and LDL cholesterol – Not improved glycemic control (absolute A 1 C reduction 0. 11%, P = 0. 42)

Metformin Adverse effects: • Common: Nausea, vomiting, diarrhea, gas, upset stomach, metallic taste (especially early) • Weight loss • Uncommon: Macrocytic anemia (caused by vitamin B 12 deficiency); lactic acidosis (uncommon but life threatening! Use only in appropriate patients) Contraindications: • Serum creatinine of 1. 5 mg/d. L or greater in men; serum creatinine of 1. 4 mg/d. L or greater in women • Creatinine clearance less than 30 m. L/minute • Severe hepatic, pulmonary, or cardiac disease • Hold for 24 hours before procedures using contrast dye • Excessive alcohol intake • Hypoxemia, dehydration, or sepsis 24

อาการไมพงประสงค • คลนไสอาเจยน • ปวดทอง ทองเสย ทองผก • hypoglycemia • แกไขโดย – กนหลงอาหา รทนทชวย ได – อมลกอมหร อผสมนำหว านจบบรรเทา อาการนำตา ลในเลอดต ำ

MALA (Metformin-associated Lactic Acidosis) เกดนอยแตรนแรง

• MALA พบประมาณ 2 -9 คน/100, 000 คน/ป • มโอกาสเสยชวต 30 -50% • ตรวจพบปรมาณ lactate ในเลอด > 5 mmol/L และคา PH ในเลอด < 7. 35 • คลนไส /อาเจยน หายใจเรว ปวดทอง ซม , หมดสต ความดนโลหตตำ หวใจเตนเรว , หวใจเตนผดจงหวะ • ปจจยเสยงททำใหเกด MALA เชน การไดรบ metformin ในปรมาณตอวนสงกวา 2, 500 mg (เมดละ 500 mg) หรอขนาด 2, 550 mg (เมดละ 850 mg), ผปวยสงอาย ,
Alpha-glucosidase Inhibitor
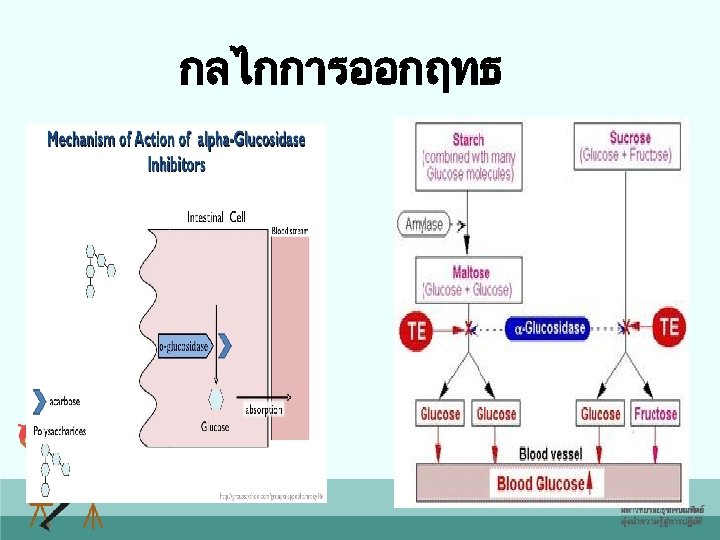
กลไกการออกฤทธ

α-Glucosidase inhibitors • Inhibits the enzyme α-glucosidase, found along the brush border of the small intestine, which is responsible for the breakdown of complex carbohydrates into glucose, thus delaying and reducing post-meal carbohydrate absorption and postprandial blood glucose • Hemoglobin A 1 C reduction of 0. 5%– 1% • Reduces postprandial blood glucose • Mealtime dosing 30

α-Glucosidase Inhibitors • Efficacy: – Lowers Hg. A 1 C ~ 0. 7 - 1% – Better post-prandial blood glucose control but fasting glucose levels are relatively unchanged – Better with starchy, high fiber diets 31

α-Glucosidase inhibitors • Acarbose(Glucobay) : 25 mg with first bite of meal; start every day and then increase weekly to 2 times/day; then 3 times/day with meals to decrease GI adverse effects (Maximal daily dose: 300 mg) • Miglitol(Glyset) : 25 mg with first bite of meal • Voglibose(Basen): 0. 2 -0. 3 mg with first bite of meal (Maximal daily dose: 0. 9 mg) • Initiate at very low dose and increase gradually over months • Skip if meal skipped 32

α-Glucosidase Inhibitors • Possible side effects: – Flatulence – Abdominal pain – Upset stomach – Diarrhea – May diminish after 4– 8 weeks of therapy – Increased liver enzymes observed with high doses of acarbose 33

α-Glucosidase Inhibitors • Warnings and Precautions: – Gastrointestinal disorders (Irritable Bowel Disease, bowel obstruction, colon ulcerations, malabsorption etc) – Liver disease (potential hepatotoxicity) – Creatinine clearance less than 25 m. L/minute or serum creatinine greater than 2 mg/d. L 34

Thiazodinedione
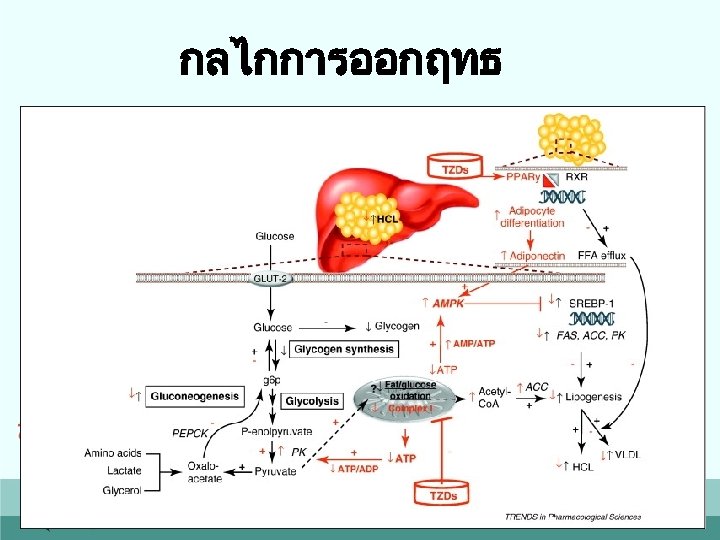
กลไกการออกฤทธ

Thiazolidinediones • Often called TZDs or glitazones • Peroxisome proliferator-activated receptor (PPAR) gamma agonist (found in adipose tissue, skeletal muscle, and the liver) • Increase in insulin-dependent glucose disposal (insulin sensitivity) in skeletal muscle and adipocytes (primarily) and a decrease in hepatic glucose production (secondarily) • Rosiglitazone and Pioglitazone 37

Thiazolidinediones • Efficacy: – Lowers Hg. A 1 C ~ 0. 5 – 1. 5% – Decreases FPG ~ 50 -80 mg/dl – Only effective in the presence of insulin • Both drugs increase HDL-C, but pioglitazone has a more favorable effect in reducing LDL-C • Onset: 4 weeks and maximum benefit in 2 -3 months 38

Thiazolidinediones • Pioglitazone(Actos) – Initial: 15 mg once daily – Maximal daily dose: 45 mg • Rosiglitazone(Avandia) – Initial: 1– 2 mg once daily – Maximal daily dose: 8 mg • Dose titration is slower with these agents, and the maximal effect of a dose change may not be observed for 8– 12 weeks 39

Thiazolidinediones • Possible side effects: – Edema (particularly peripheral edema) – Weight gain – Headache, Weakness – Nausea, vomiting, abdominal pain – Bone fracture – Increase the risk of heart failure – Liver problems (RARE) – Pioglitazone associated with small risk of bladder cancer – Potential myocardial infarctions (rosiglitazone) 40

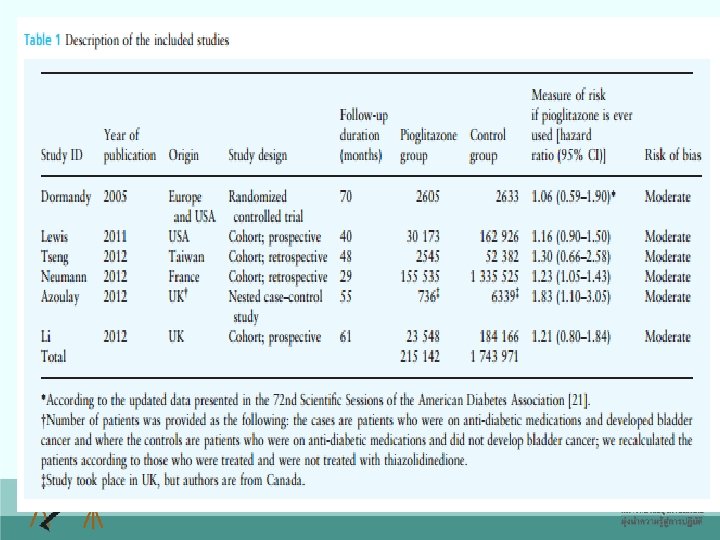

Thiazolidinediones • Contraindications: – Active liver disease; LFTs >2. 5 times ULN – Type 1 diabetes (ineffective without insulin) – Diabetic ketoacidosis – Heart Failure - NYHA class III or IV (causes plasma volume expansion) 43

ควรตรวจวดการทำงานของตบกอน เรมยา และในชวงรกษา หากคาการเอนไซมของตบขนมา กกวา 2 เทาของคาปกตควรหยดยา
DPP-4 inhibitor (Dipeptidyl Peptidase Inhibitor-4)
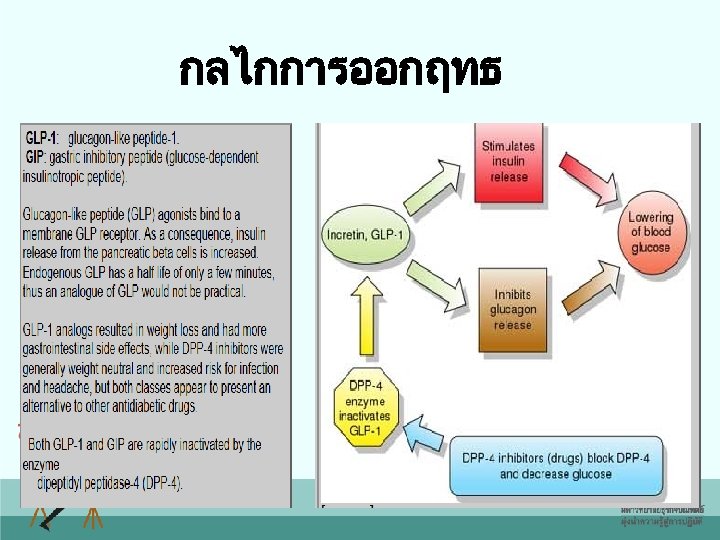
กลไกการออกฤทธ
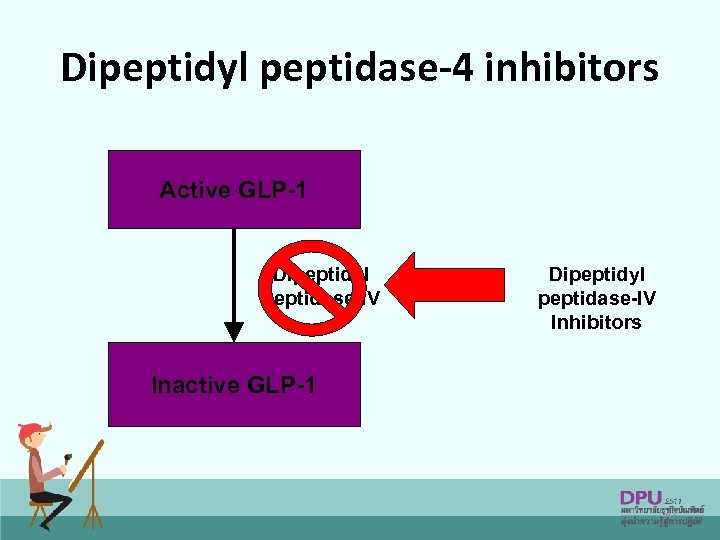
Dipeptidyl peptidase-4 inhibitors Active GLP-1 Dipeptidyl peptidase-IV Inhibitors Inactive GLP-1 47

Dipeptidyl peptidase-4 inhibitors • Inhibits the enzyme dipeptidyl peptidase-4 from breaking down endogenous GLP-1 and GIP, resulting in increased endogenous incretin levels. This results in – Glucose-dependent increase in insulin secretion – Glucose-dependent inhibition of glucagon secretion 48

Dipeptidyl peptidase-4 inhibitors Hemoglobin A 1 c lowering of 0. 5%– 1. 1% Reduces primarily postprandial glucose Weight neutral Sitagliptin(Januvia) Saxagliptin(Onglyza) Vildagliptin(Galvus) Alogliptin(Nesina): 25 mg/day(Reduced in renal impairment) • Linagliptin(Trajenta): 5 mg/day(No dose adjustment in renal impairment) • • 49
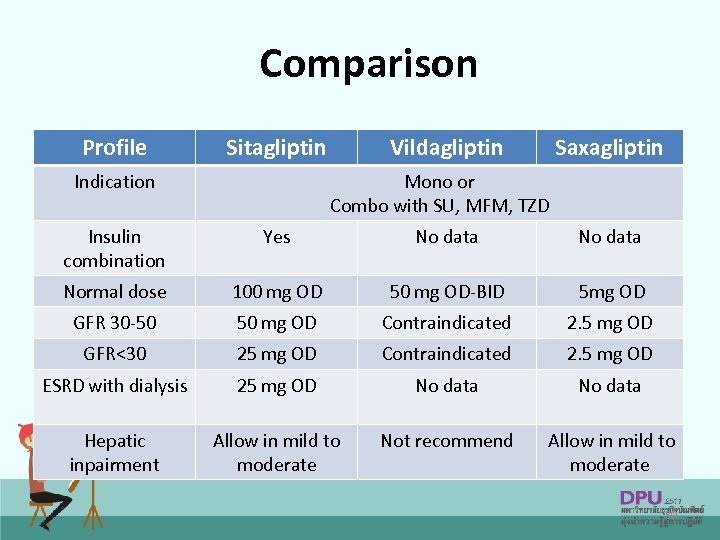
Comparison Profile Sitagliptin Indication Vildagliptin Saxagliptin Mono or Combo with SU, MFM, TZD Insulin combination Yes No data Normal dose 100 mg OD 50 mg OD-BID 5 mg OD GFR 30 -50 50 mg OD Contraindicated 2. 5 mg OD GFR<30 25 mg OD Contraindicated 2. 5 mg OD ESRD with dialysis 25 mg OD No data Hepatic inpairment Allow in mild to moderate Not recommend Allow in mild to moderate 50

Dipeptidyl peptidase-4 inhibitors • Contraindications: • Adverse effects: – History of pancreatitis – Diabetic ketoacidosis – Type 1 DM – Placebo-like incidence of adverse effects (URI, headache, UTI) – Hypoglycemia with monotherapy is minimal, but increased frequency with concurrent sulfonylurea therapy – Sitagliptin has had some postmarketing reports of acute pancreatitis, angioedema, Stevens-Johnson syndrome, and anaphylaxis 51

The Kidneys Play an Important Role in Glucose Control Normal Renal Glucose Physiology • 180 g of glucose is filtered each day • Virtually all glucose reabsorbed in the proximal tubules & reenters the circulation • SGLT 2 reabsorbs about 90% of the glucose • SGLT 1 reabsorbs about 10% of the glucose • Virtually no glucose excreted in urine Mather, A & Pollock, C. Kidney International. 2011; 79: S 1 -S 6.
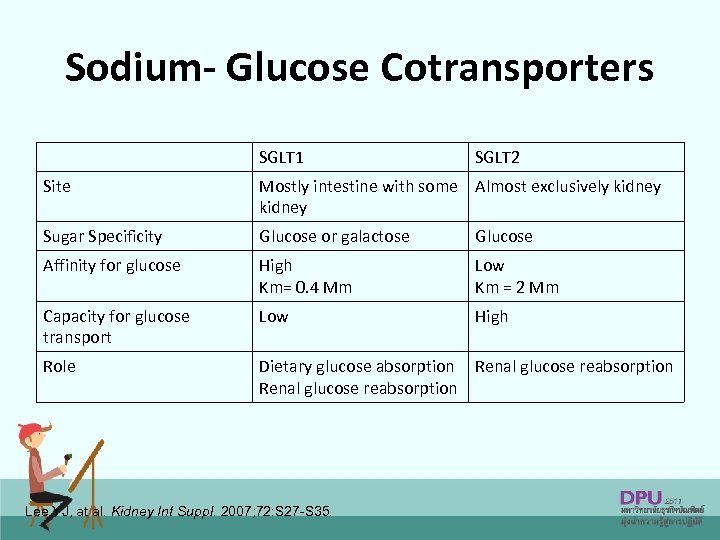
Sodium- Glucose Cotransporters SGLT 1 SGLT 2 Site Mostly intestine with some Almost exclusively kidney Sugar Specificity Glucose or galactose Glucose Affinity for glucose High Km= 0. 4 Mm Low Km = 2 Mm Capacity for glucose transport Low High Role Dietary glucose absorption Renal glucose reabsorption Lee YJ, at al. Kidney Int Suppl. 2007; 72: S 27 -S 35.
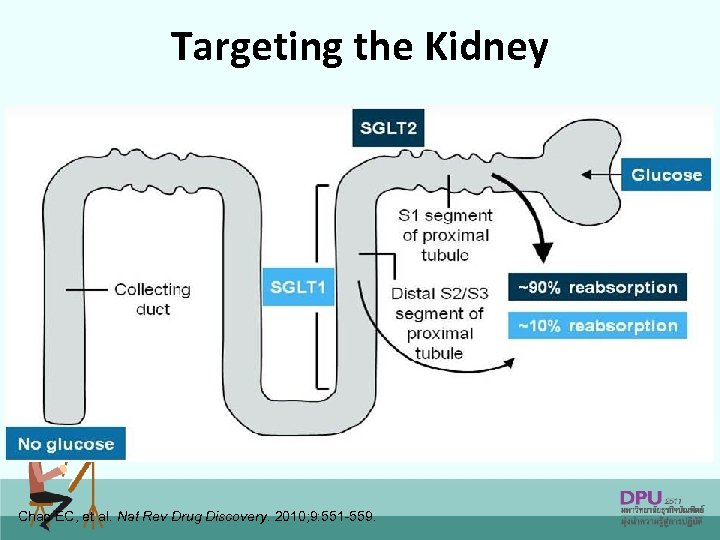
Targeting the Kidney Chao EC, et al. Nat Rev Drug Discovery. 2010; 9: 551 -559.
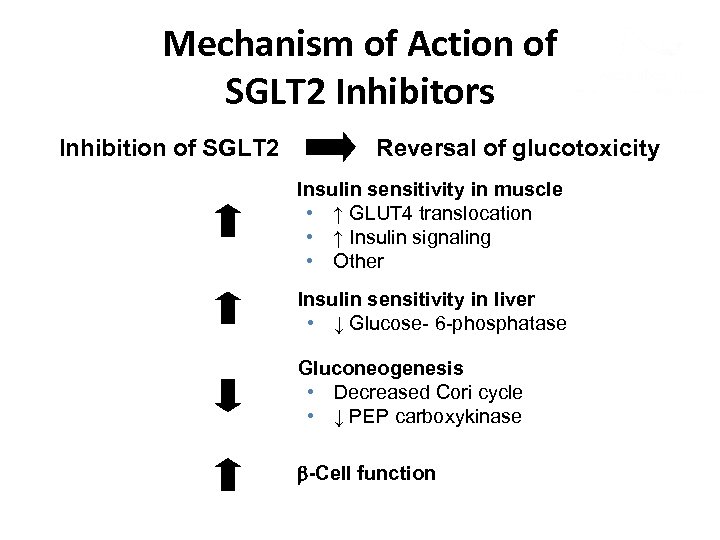
Mechanism of Action of SGLT 2 Inhibitors Inhibition of SGLT 2 Reversal of glucotoxicity Insulin sensitivity in muscle • ↑ GLUT 4 translocation • ↑ Insulin signaling • Other Insulin sensitivity in liver • ↓ Glucose- 6 -phosphatase Gluconeogenesis • Decreased Cori cycle • ↓ PEP carboxykinase -Cell function

SGLT 2 Inhibitors Dapagliflozin(Farxiga) : 5 -10 mg daily Canagliflozin(Invokana): 100 -300 mg daily Reducing A 1 C by 0. 55%– 0. 89% The long-term safety of this class remains to be proven • Risk of nocturia and genitourinary infections may limit use in some patients • SGLT 2 inhibition may not be effective in patients with renal impairment • • 56

Perspectives on SGLT 2 Inhibition • Potential advantages • Concerns – Insulin Independence – Weight loss (75 g urine glucose = 300 kcal/day) – Low risk of hypoglycemia – Blood pressure lowering? – Polyuria – Electrolyte disturbances – Bacterial urinary tract infections – Fungal genital infections – Malignancies
Insulin • ใชลดระดบนำตาลในเลอดในผปวยเ บาหวานชนดท 1 และ 2
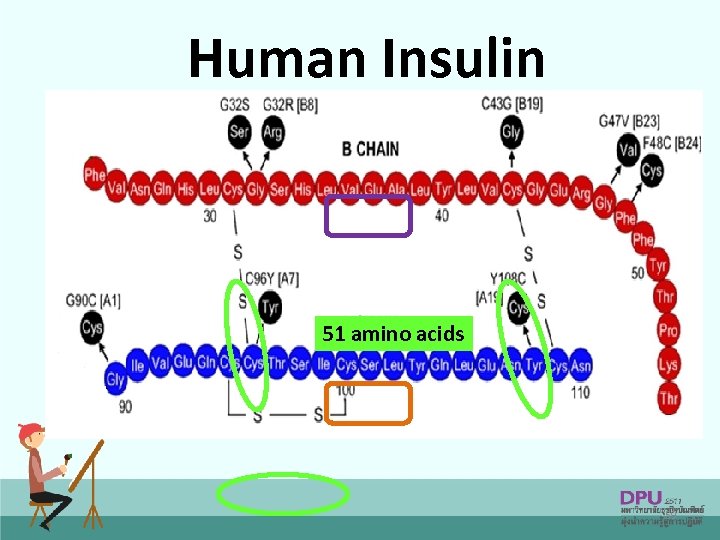
Human Insulin 51 amino acids 59
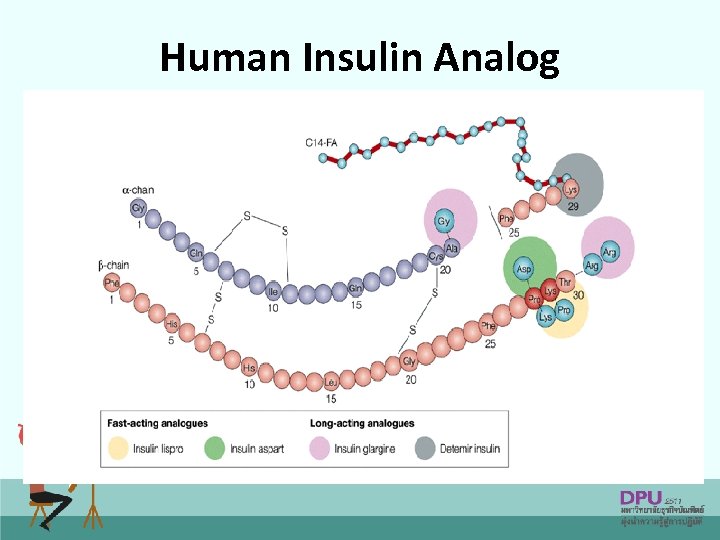
Human Insulin Analog
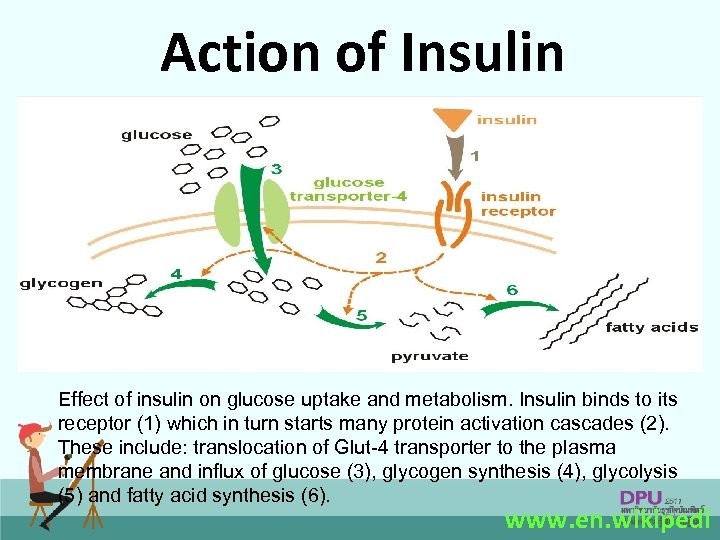
Action of Insulin Effect of insulin on glucose uptake and metabolism. Insulin binds to its receptor (1) which in turn starts many protein activation cascades (2). These include: translocation of Glut-4 transporter to the plasma membrane and influx of glucose (3), glycogen synthesis (4), glycolysis (5) and fatty acid synthesis (6). 61 www. en. wikipedi

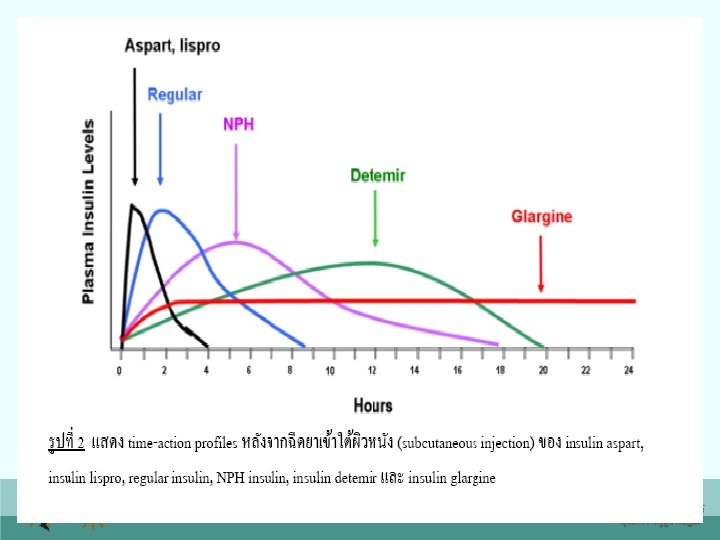
Insulin classification Rapid acting insulin: Aspart, Lispro Short acting insulin: Regular Intermediate acting insulin: NPH, Lente Long acting insulin: Ultralente, Glargine, Detemir 62

Insulin Fixed - Mix products • Advantages – “Easy” to use – usually two injections per day – Not necessary to mix prior to administering (already mixed) – Available in insulin pens 63

Insulin’s Pharmacokinetics • Distribution: throughtout the extracellulars fluids, no plasma protein binding • Metabolism: mainly in the liver • Excretion: filtered through the glomeruli and completely(98%) reabsorbed in the proximal tubules 64
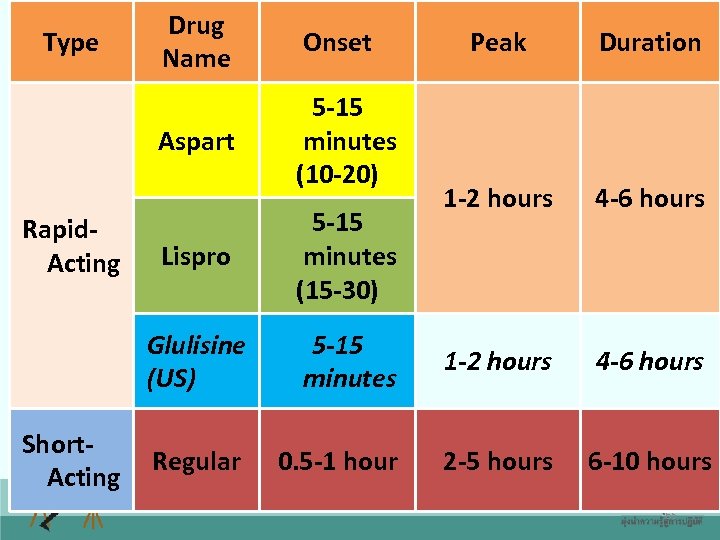
Onset Aspart Type Drug Name 5 -15 minutes (10 -20) Peak Duration 1 -2 hours 4 -6 hours Short. Acting Lispro 5 -15 minutes (15 -30) Glulisine (US) Rapid. Acting 5 -15 minutes 1 -2 hours 4 -6 hours Regular 0. 5 -1 hour 2 -5 hours 6 -10 hours 65
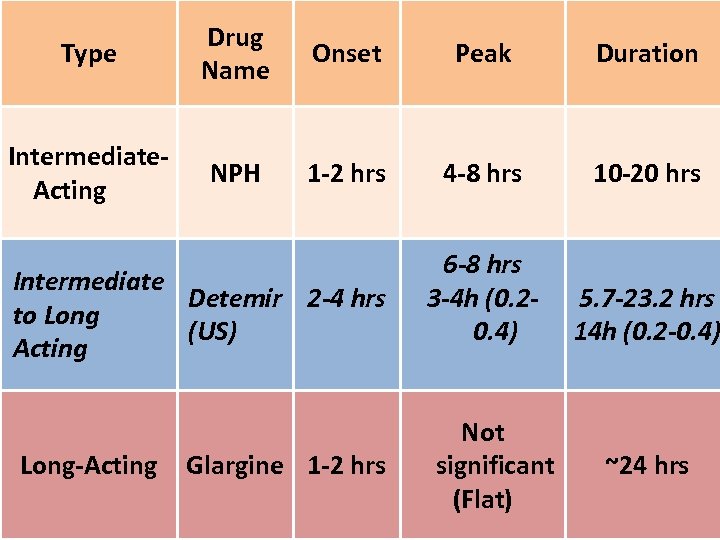
Type Drug Name Onset Peak Duration Intermediate. Acting NPH 1 -2 hrs 4 -8 hrs 10 -20 hrs 6 -8 hrs 3 -4 h (0. 20. 4) 5. 7 -23. 2 hrs 14 h (0. 2 -0. 4) Intermediate Detemir 2 -4 hrs to Long (US) Acting Long-Acting Glargine 1 -2 hrs Not significant (Flat) ~24 hrs 66
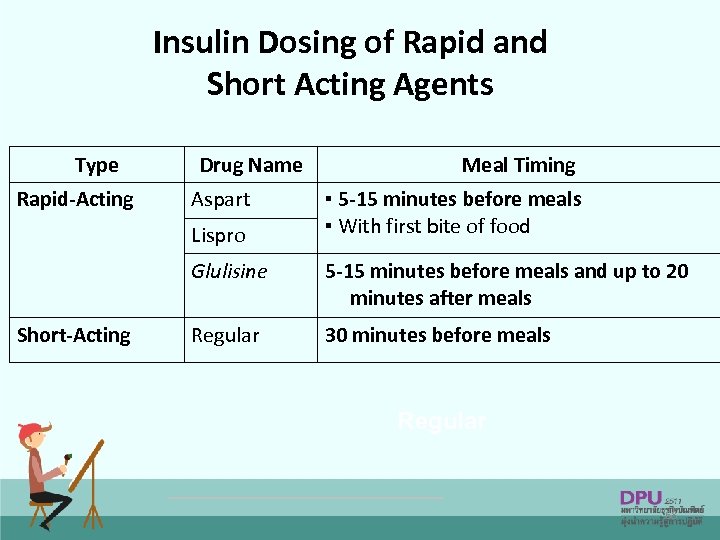
Insulin Dosing of Rapid and Short Acting Agents Type Rapid-Acting Drug Name Aspart Lispro Meal Timing ▪ 5 -15 minutes before meals ▪ With first bite of food Glulisine Short-Acting 5 -15 minutes before meals and up to 20 minutes after meals Regular 30 minutes before meals Regular 68
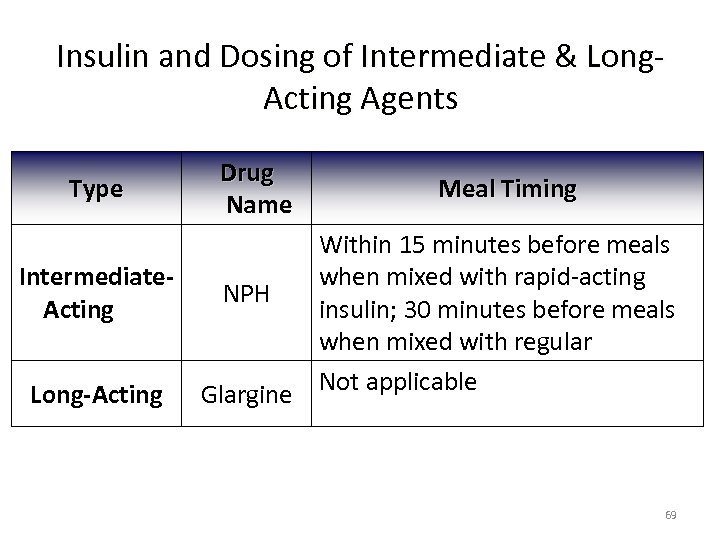
Insulin and Dosing of Intermediate & Long. Acting Agents Type Drug Name Meal Timing Within 15 minutes before meals Intermediatewhen mixed with rapid-acting NPH Acting insulin; 30 minutes before meals when mixed with regular Long-Acting Glargine Not applicable 69

รปแบบการใหบรหารอนซลน ใน ผปวยเบาหวาน type 2 • Basal insulin รกษาระดบกลโคสใหคงท – ให NPH หรอ Lante เชาและกอนนอน – Continuous subcutaneous insulin infusion (CSII) – Insulin gargline วนละ 1 -2 ครง • Prandial insulin หลงออกมาเพอนำกลโคสเขาไปในเซลล + ยบยงการปลดปลอยกลโคสจากตบ – Insulin aspart, insulin lispro หรอ regular insulin กอนอาหารทกมอ • Correction-dose insulin

วธการบรหารอนซลน • One daily insulin regimen – ให NPH หรอ insulin gargline หรอ pre-mixed insulin 70/30 มอกอนนอน • Multiple dose insulin injection (MDI) – ให regular insulin หรอ aspart หรอ lispro กอนอาหารทกมอ + intermediate insulin เชาและกอนนอน • Split and mixed insulin regimen – ใหอนซลนวนละ 2 มอ โดยให intermediate insulin + regular insulin หรอ aspart

วธการบรหารอนซลน • Split and mixed insulin program with bedtime intermediate insulin – ฉด intermediate insulin + regular or insulin analog เชา และ ฉด regular or insulin analog และ ฉด intermediate insulin กอนนอน • continuous subcutaneous insulin infusion (CSII) ใชเครองชวยผลก rapid-acting insulin analog เขาสรางกายตลอดเวลา • Intravenous insulin infusion
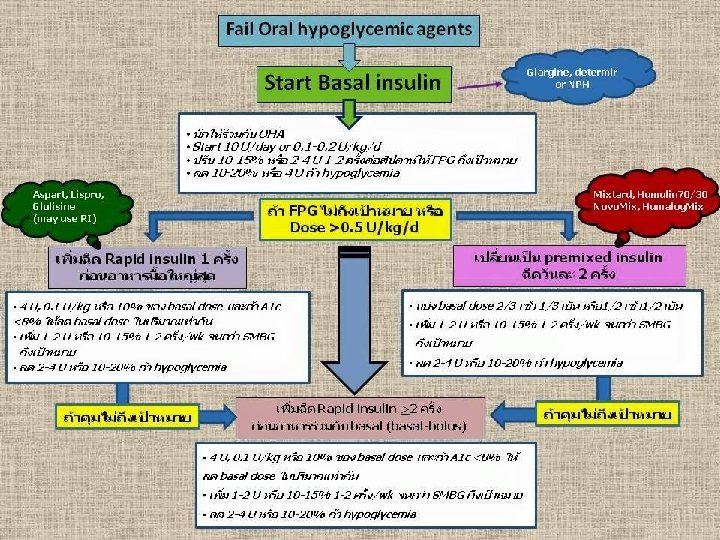
73

Morning hyperglycaemia Feature comparing Dawn phenomenon Somogyi effect Definition Recurring early morning hyperglycaemia Early morning hyperglycaemia due to treatment with excessive amount of exogenous insulin Cause Diagnosis (3 a. m. and 5 a. m. glucose level) Decrease of insulin Nocturnal hypoglycemia secretion between 3 a. m. due to excessive dose of and insulin 5 a. m. High/normal plasma glucose level Low plasma glucose level 74

Morning hyperglycaemia Dawn phenomenon • Increase insulin dose before bedtime • Long-acting insulin analogues Somogyi effect • Shift RI to NPH before bedtime • Decrease insulin dose before bedtime • Long-acting insulin analogues • Go to bed with higher level of plasma glucose than usual 75
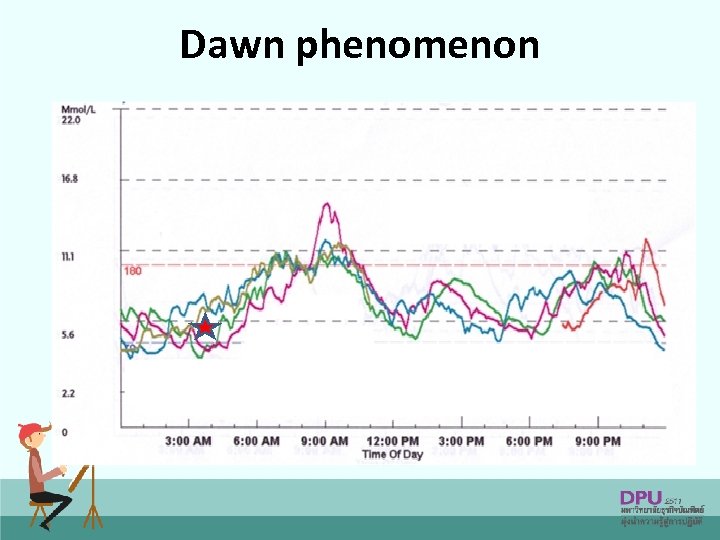
Dawn phenomenon
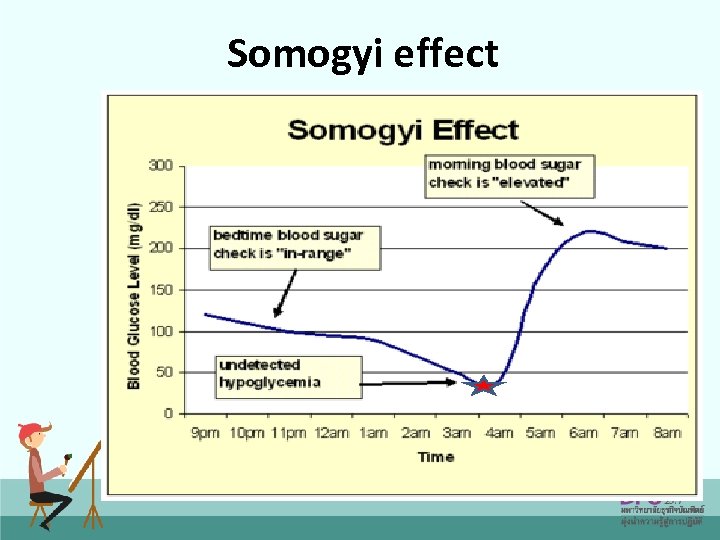
Somogyi effect
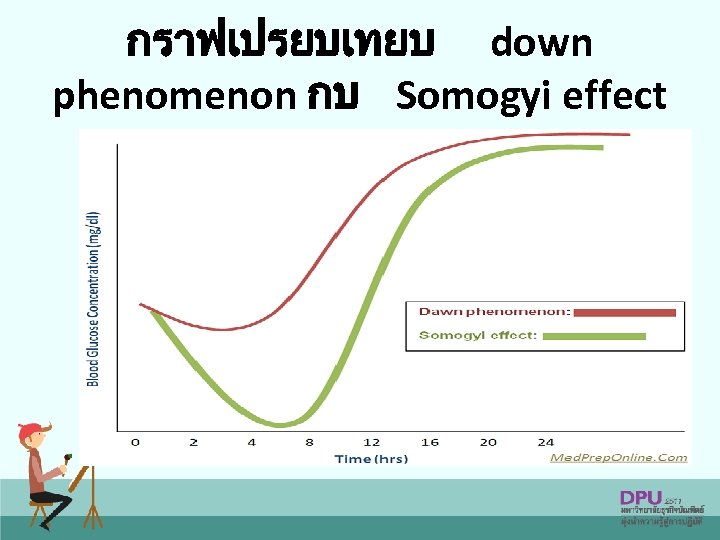
กราฟเปรยบเทยบ down phenomenon กบ Somogyi effect
Insulin inj (vial)
Novomix flexpen (Insulin Aspart) Insulin gargline
Penfill
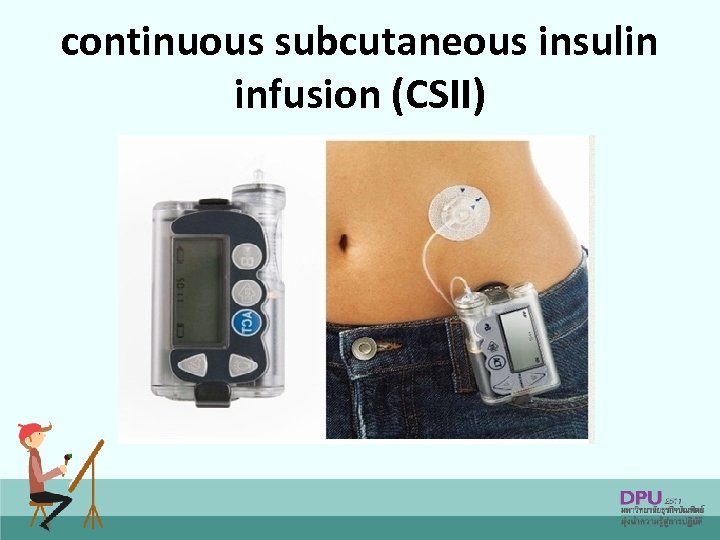
continuous subcutaneous insulin infusion (CSII)

Insulin storage & Shelf life Storage -Unopened: 2 -8๐ C -Opened: <30๐ C Shelf life -Unopened: (2 -8๐ C) until expired date (15 -30๐ C) 28 days -Opened: 28 days (independ on temperature) 83

Adverse Reactions of Insulin • Possible Side Effects: – Low blood sugar (Hypoglycemia) – Weight gain – Injection site reaction 84
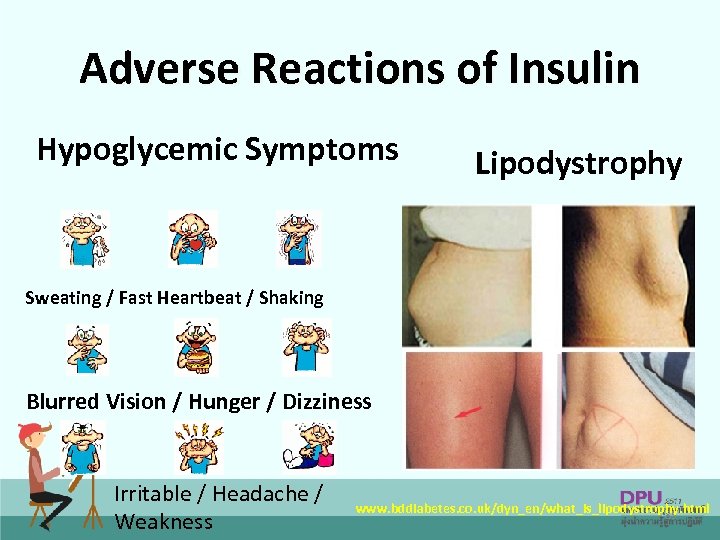
Adverse Reactions of Insulin Hypoglycemic Symptoms Lipodystrophy Sweating / Fast Heartbeat / Shaking Blurred Vision / Hunger / Dizziness Irritable / Headache / Weakness www. bddiabetes. co. uk/dyn_en/what_is_lipodystrophy. html 85

When can Hypoglycemia occur? • • • Eat too little food Delay or skip a meal or snack Exercise harder or longer than usual Take too much medicine or insulin Sickness Drink alcohol on an empty stomach 86

Diabetes Checklist 1. Hemoglobin A 1 c of 7% or less (6. 5%) (not consistent with goals listed above) 2. Blood pressure 140/80 mm Hg or less (ACEI/ARB) 3. Low-density lipoprotein cholesterol of 100 (70) mg/d. L or less (statin) 4. Daily ASA use for vascular protection 5. Smoking cessation 6. Immunizations (influenza, pneumococcal, HBV) 87

Diabetes Checklist 7. Urinalysis 8. Daily feet inspection 9. Annual dilated eye examinations 10. Realistic exercise program 11. Weight loss (5%– 10%) 12. Dental examinations (peridontal disease) 88
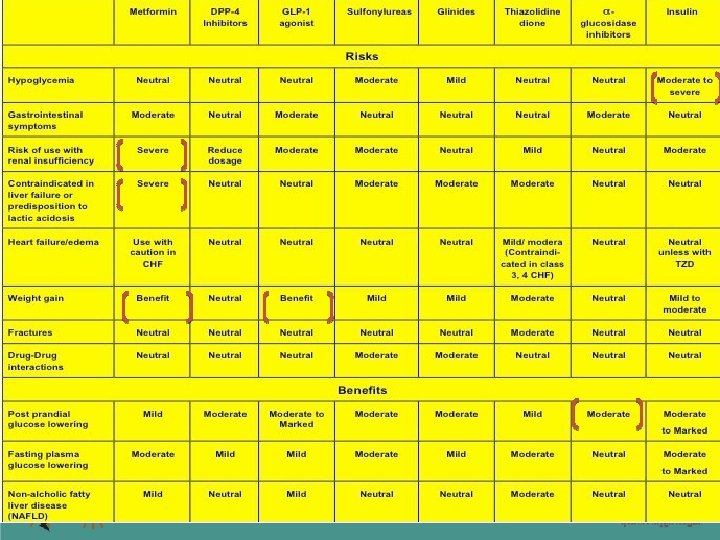
89

Thank you
658a5b2dc3c37bfbee9a8e29ebd1c516.ppt