Презентация Water Salt Balance 2008



















- Размер: 8.3 Mегабайта
- Количество слайдов: 42
Описание презентации Презентация Water Salt Balance 2008 по слайдам
 Metabolic disorders Part 3 07. 12.
Metabolic disorders Part 3 07. 12.
 Typical mechanisms of carbohydrate metabolism disorders 1. Disorders of digestion and absorption 2. Disorders of the gluconeogenesis and glycolysis 3. Altered synthesis and breakdown of glycogen (glycogenoses) 4. Disorders of glucose uptake by the cells 5. Hypoglycemia, hyperglycemia
Typical mechanisms of carbohydrate metabolism disorders 1. Disorders of digestion and absorption 2. Disorders of the gluconeogenesis and glycolysis 3. Altered synthesis and breakdown of glycogen (glycogenoses) 4. Disorders of glucose uptake by the cells 5. Hypoglycemia, hyperglycemia
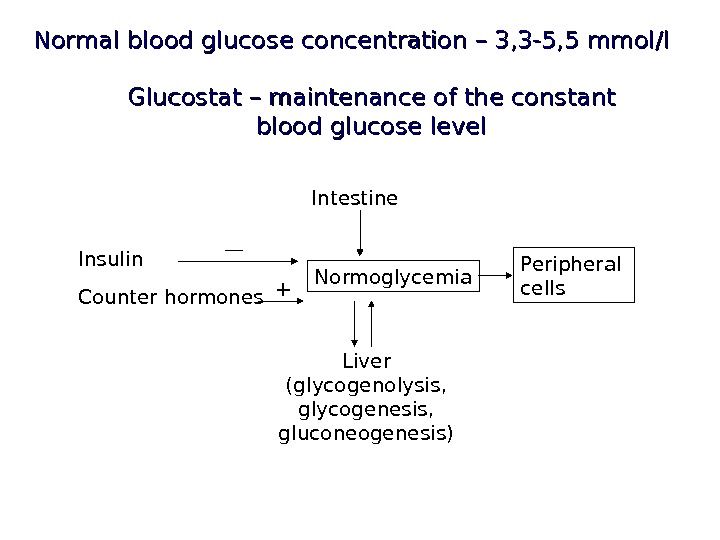
 Normal blood glucose concentration – 3, 3 -5, 5 mmol/l Normoglycemia Peripheral cells. Intestine Liver ( glycogenolysis , glycogenesis, gluconeogenesis )Insulin Counter hormones — +Glucostat – maintenance of the constant blood glucose level
Normal blood glucose concentration – 3, 3 -5, 5 mmol/l Normoglycemia Peripheral cells. Intestine Liver ( glycogenolysis , glycogenesis, gluconeogenesis )Insulin Counter hormones — +Glucostat – maintenance of the constant blood glucose level
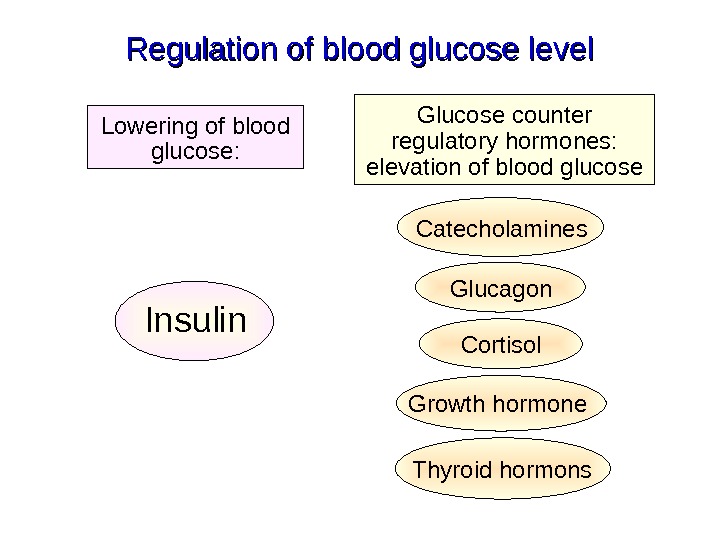
 Regulation of blood glucose level Glucose counter regulatory hormones: elevation of blood glucose. Lowering of blood glucose: Insulin Catecholamines Glucagon Cortisol Growth hormone Thyroid hormons
Regulation of blood glucose level Glucose counter regulatory hormones: elevation of blood glucose. Lowering of blood glucose: Insulin Catecholamines Glucagon Cortisol Growth hormone Thyroid hormons
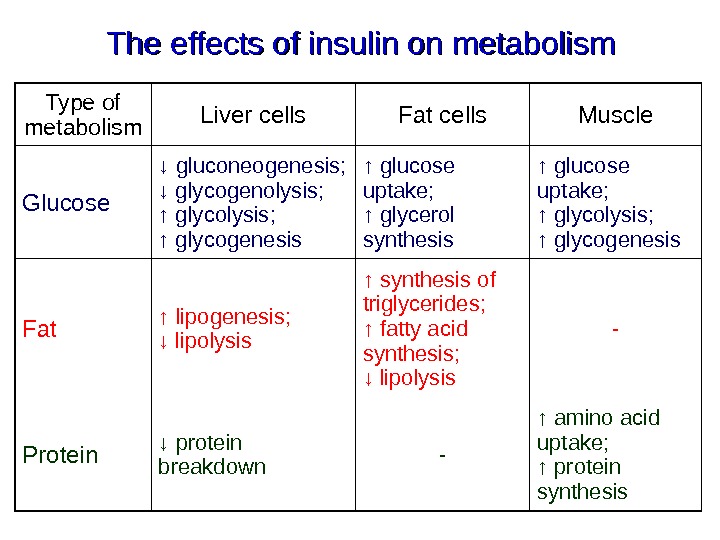
 The effects of insulin on metabolism Type of metabolism Liver cells Fat cells Muscle Glucose ↓ gluconeogenesis; ↓ glycogenolysis; ↑ glycolysis; ↑ glycogenesis ↑ glucose uptake; ↑ glycerol synthesis ↑ glucose uptake; ↑ glycolysis; ↑ glycogenesis Fat ↑ lipogenesis; ↓ lipolysis ↑ synthesis of triglycerides; ↑ fatty acid synthesis; ↓ lipolysis — Protein ↓ protein breakdown — ↑ amino acid uptake; ↑ protein synthesis
The effects of insulin on metabolism Type of metabolism Liver cells Fat cells Muscle Glucose ↓ gluconeogenesis; ↓ glycogenolysis; ↑ glycolysis; ↑ glycogenesis ↑ glucose uptake; ↑ glycerol synthesis ↑ glucose uptake; ↑ glycolysis; ↑ glycogenesis Fat ↑ lipogenesis; ↓ lipolysis ↑ synthesis of triglycerides; ↑ fatty acid synthesis; ↓ lipolysis — Protein ↓ protein breakdown — ↑ amino acid uptake; ↑ protein synthesis
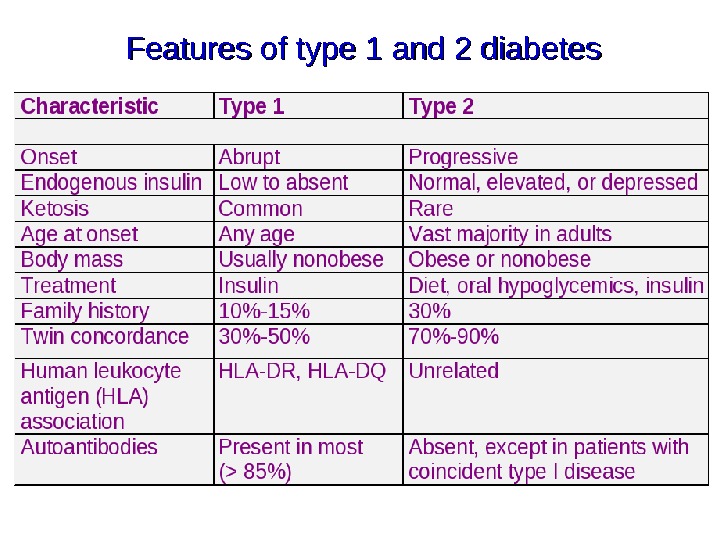
 Features of type 1 and 2 diabetes
Features of type 1 and 2 diabetes
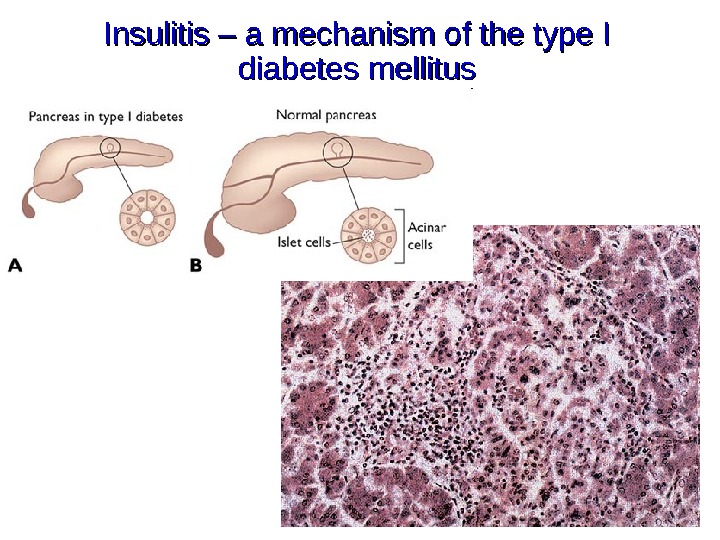
 Insulitis – a mechanism of the type I diabetes mellitus
Insulitis – a mechanism of the type I diabetes mellitus
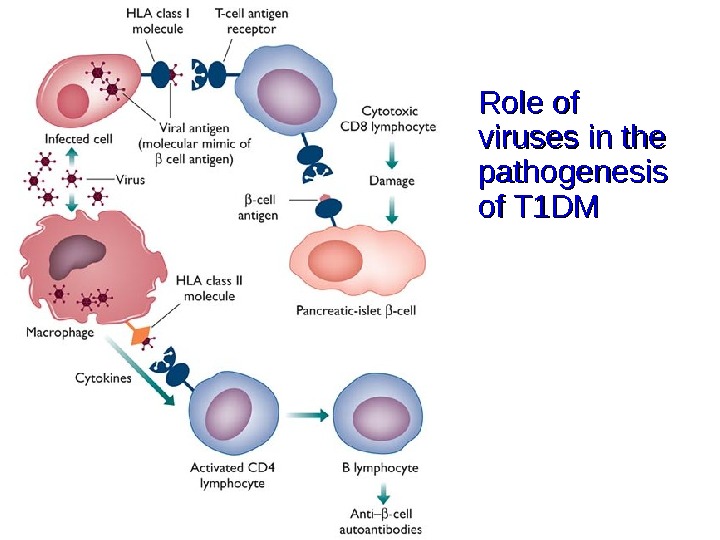
 Role of viruses in the pathogenesis of T 1 DM
Role of viruses in the pathogenesis of T 1 DM
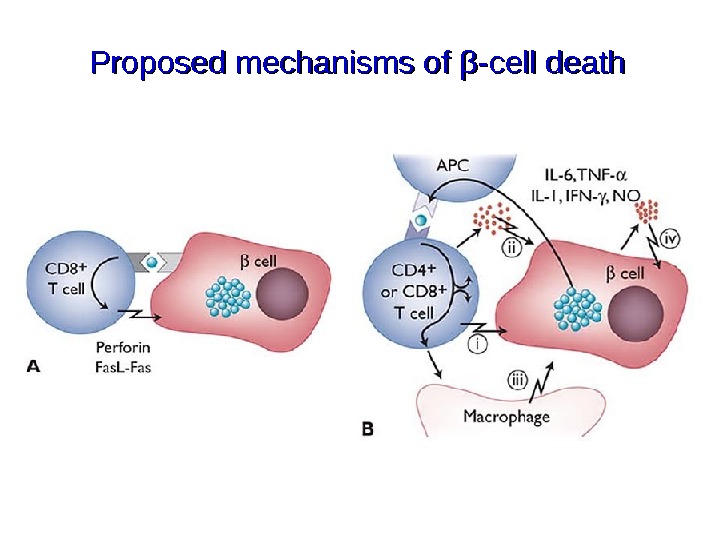
 Proposed mechanisms of ββ -cell death
Proposed mechanisms of ββ -cell death
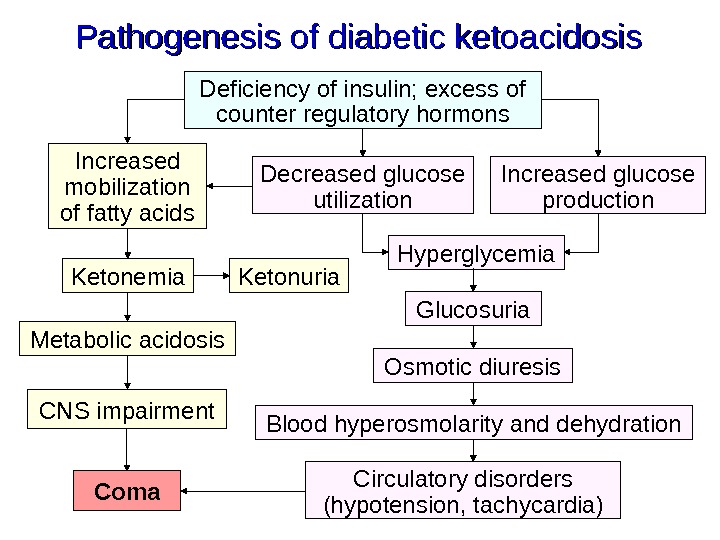
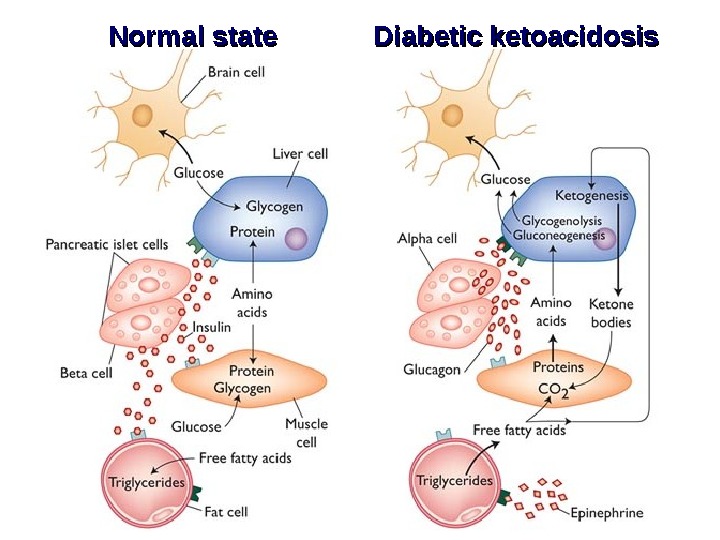
 Pathogenesis of diabetic ketoacidosis Deficiency of insulin; excess of counter regulatory hormons Decreased glucose utilization Increased glucose production. Increased mobilization of fatty acids Ketonemia Ketonuria Hyperglycemia Glucosuria Osmotic diuresis Blood hyperosmolarity and dehydration. Metabolic acidosis CNS impairment Circulatory disorders (hypotension, tachycardia)Coma
Pathogenesis of diabetic ketoacidosis Deficiency of insulin; excess of counter regulatory hormons Decreased glucose utilization Increased glucose production. Increased mobilization of fatty acids Ketonemia Ketonuria Hyperglycemia Glucosuria Osmotic diuresis Blood hyperosmolarity and dehydration. Metabolic acidosis CNS impairment Circulatory disorders (hypotension, tachycardia)Coma
 Normal state Diabetic ketoacidosis
Normal state Diabetic ketoacidosis
 Pathogenesis of T 2 DM
Pathogenesis of T 2 DM
 1. Prereceptor level ( anomalous insulin ) 2. Receptor level ( decreased number of insulin receptors, decreased affinity of the receptors ) 3. At the level of glucose transport ( decreased number of GLUT) 4. Postreceptor level ( disorders of signal transduction and kinase phosphorylation )Mechanisms of insulin resistance
1. Prereceptor level ( anomalous insulin ) 2. Receptor level ( decreased number of insulin receptors, decreased affinity of the receptors ) 3. At the level of glucose transport ( decreased number of GLUT) 4. Postreceptor level ( disorders of signal transduction and kinase phosphorylation )Mechanisms of insulin resistance
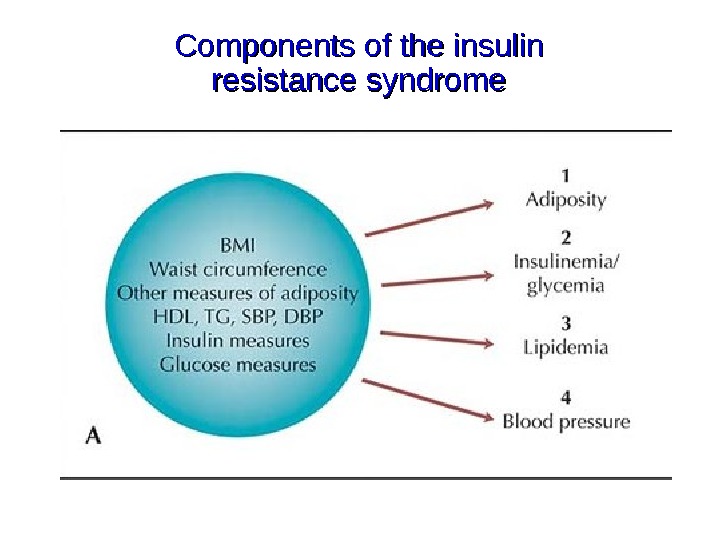
 Components of the insulin resistance syndrome
Components of the insulin resistance syndrome
 Consequences of hyperglycemia ● Glucosuria , polyuria , secondary polydipsia … ● Blood hyperosmolarity, tissue dehydration, hyperosmolar coma ● Non-enzymatic glycation of proteins (albumins, hemoglobin etc. ) – formation of advanced glycation end-products ● Endothelial dysfunction ( micro- and macroangiopathy ) ● Formation of autoantigens (autoimmune reactions)
Consequences of hyperglycemia ● Glucosuria , polyuria , secondary polydipsia … ● Blood hyperosmolarity, tissue dehydration, hyperosmolar coma ● Non-enzymatic glycation of proteins (albumins, hemoglobin etc. ) – formation of advanced glycation end-products ● Endothelial dysfunction ( micro- and macroangiopathy ) ● Formation of autoantigens (autoimmune reactions)
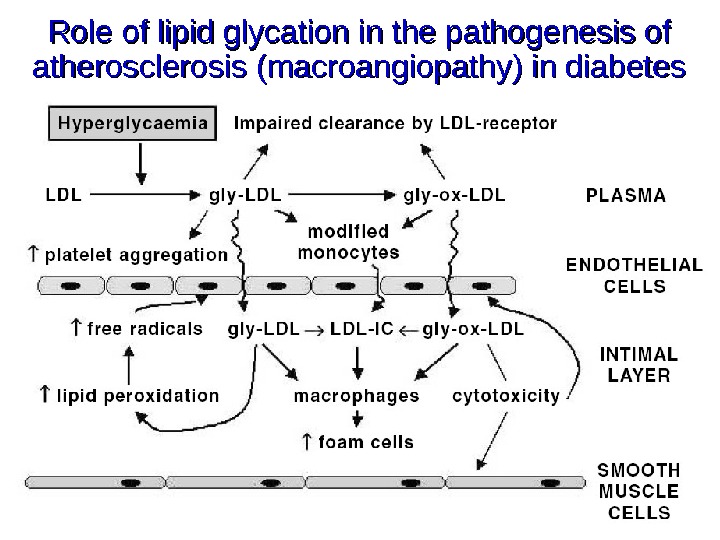
 Role of lipid glycation in the pathogenesis of atherosclerosis (macroangiopathy) in diabetes
Role of lipid glycation in the pathogenesis of atherosclerosis (macroangiopathy) in diabetes

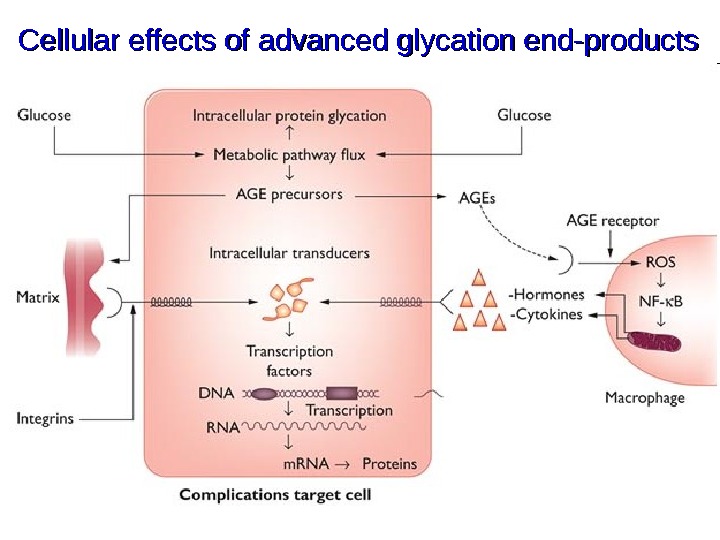
 Cellular effects of advanced glycation end-products
Cellular effects of advanced glycation end-products
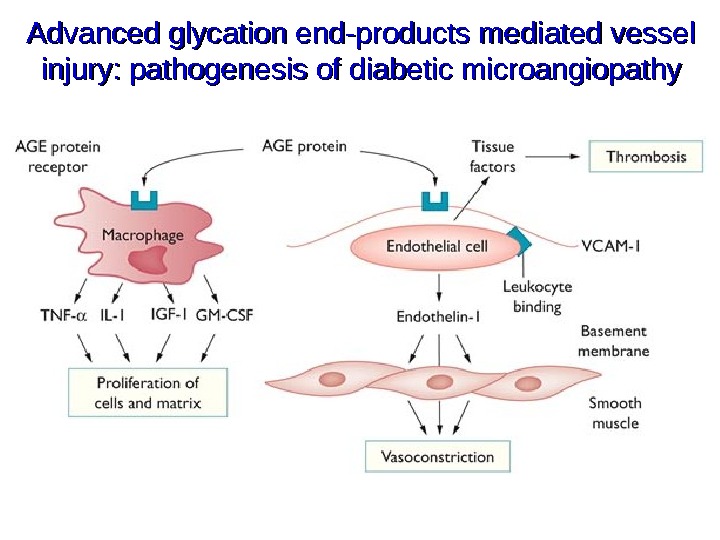
 Advanced glycation end-products mediated vessel injury: pathogenesis of diabetic microangiopathy
Advanced glycation end-products mediated vessel injury: pathogenesis of diabetic microangiopathy
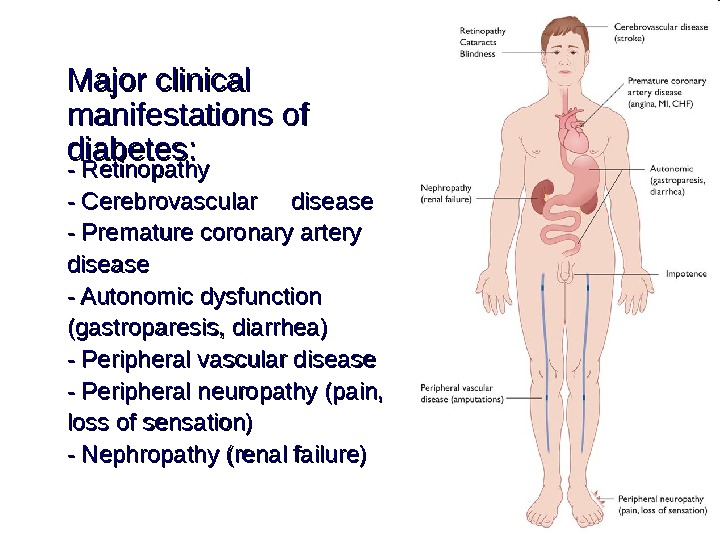
 Major clinical manifestations of diabetes: — Retinopathy — Cerebrovascular disease — Premature coronary artery disease — Autonomic dysfunction (gastroparesis, diarrhea) — Peripheral vascular disease — Peripheral neuropathy (pain, loss of sensation) — Nephropathy (( renal failure ))
Major clinical manifestations of diabetes: — Retinopathy — Cerebrovascular disease — Premature coronary artery disease — Autonomic dysfunction (gastroparesis, diarrhea) — Peripheral vascular disease — Peripheral neuropathy (pain, loss of sensation) — Nephropathy (( renal failure ))
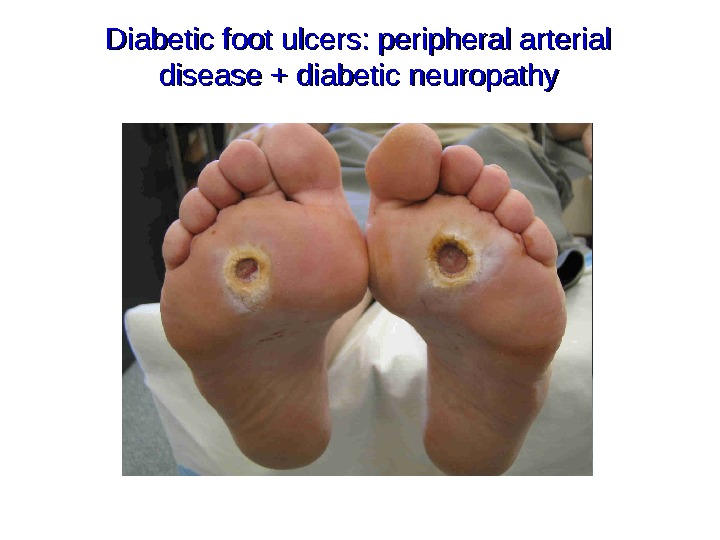
 Diabetic foot ulcers: peripheral arterial disease + diabetic neuropathy
Diabetic foot ulcers: peripheral arterial disease + diabetic neuropathy
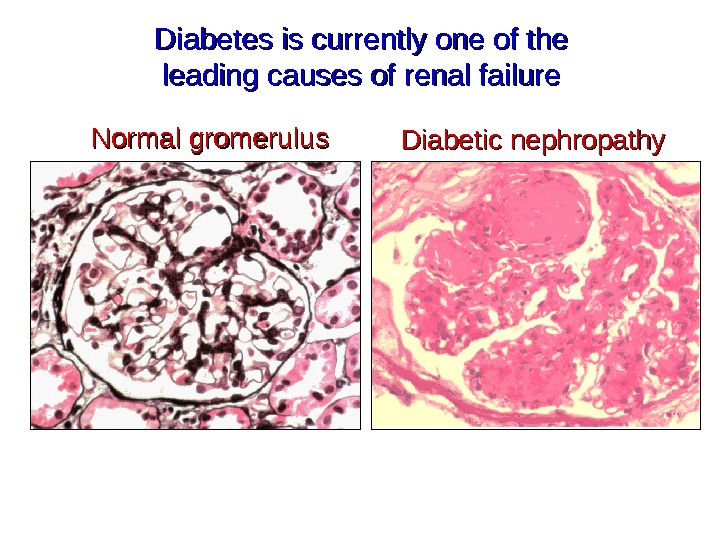
 Diabetes is currently one of the leading causes of renal failure Normal gromerulus Diabetic nephropathy
Diabetes is currently one of the leading causes of renal failure Normal gromerulus Diabetic nephropathy
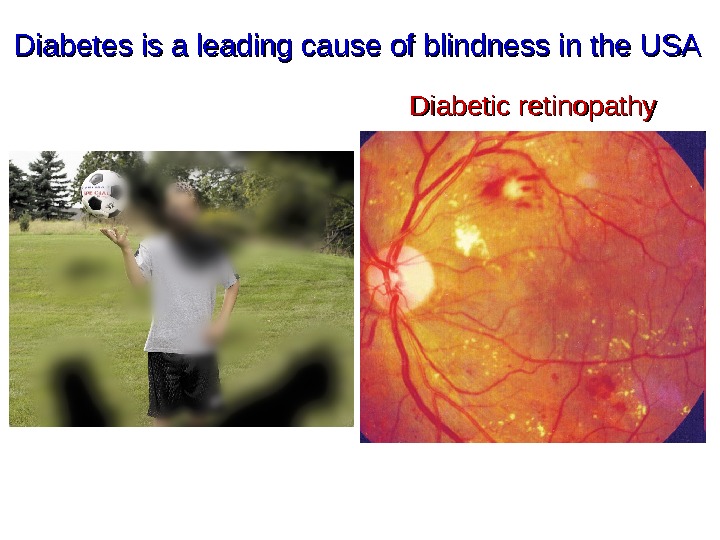
 Diabetes is a leading cause of blindness in the USA Diabetic retinopathy
Diabetes is a leading cause of blindness in the USA Diabetic retinopathy
 • Increased utilization of glucose by the cells – increased insulin production, treatment with insulin – formation of insulin-like growth factors • Disorders of glycogenolysis ( glycogenoses, liver cirrhosis ) • Disorders of glucose reabsorption ( renal diabtes ) • Prolonged intensive physical exercise Mechanisms of hypoglycemia
• Increased utilization of glucose by the cells – increased insulin production, treatment with insulin – formation of insulin-like growth factors • Disorders of glycogenolysis ( glycogenoses, liver cirrhosis ) • Disorders of glucose reabsorption ( renal diabtes ) • Prolonged intensive physical exercise Mechanisms of hypoglycemia
 Mechanisms of compensation in hypoglycemia ● Activation of sympathetic nervous system ( glycogenolysis ) ● Increased production of glucose counter regulatory hormones , gluconeogenesis , activation of lipolysis and decreased utilization of glucose
Mechanisms of compensation in hypoglycemia ● Activation of sympathetic nervous system ( glycogenolysis ) ● Increased production of glucose counter regulatory hormones , gluconeogenesis , activation of lipolysis and decreased utilization of glucose
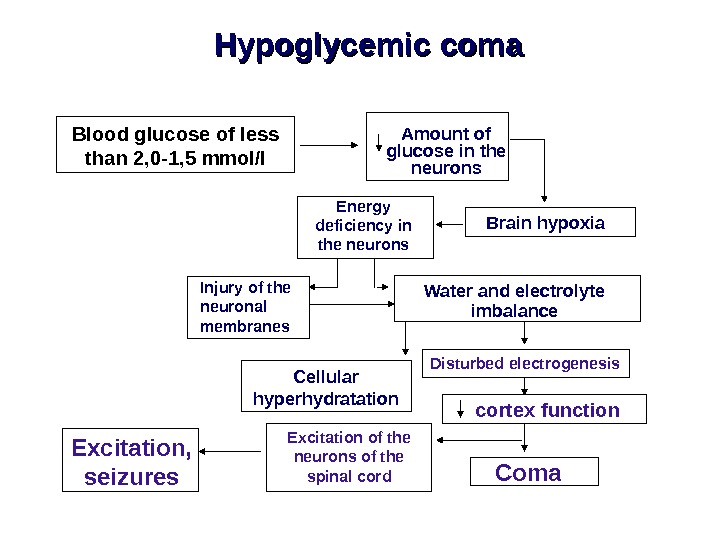
 Hypoglycemic coma Blood glucose of less than 2, 0 -1, 5 mmol/l Amount of glucose in the neurons Brain hypoxia. Energy deficiency in the neurons Water and electrolyte imbalance. Injury of the neuronal membranes Cellular hyperhydratation Disturbed electrogenesis cortex function Excitation of the neurons of the spinal cord. Excitation, seizures Coma
Hypoglycemic coma Blood glucose of less than 2, 0 -1, 5 mmol/l Amount of glucose in the neurons Brain hypoxia. Energy deficiency in the neurons Water and electrolyte imbalance. Injury of the neuronal membranes Cellular hyperhydratation Disturbed electrogenesis cortex function Excitation of the neurons of the spinal cord. Excitation, seizures Coma
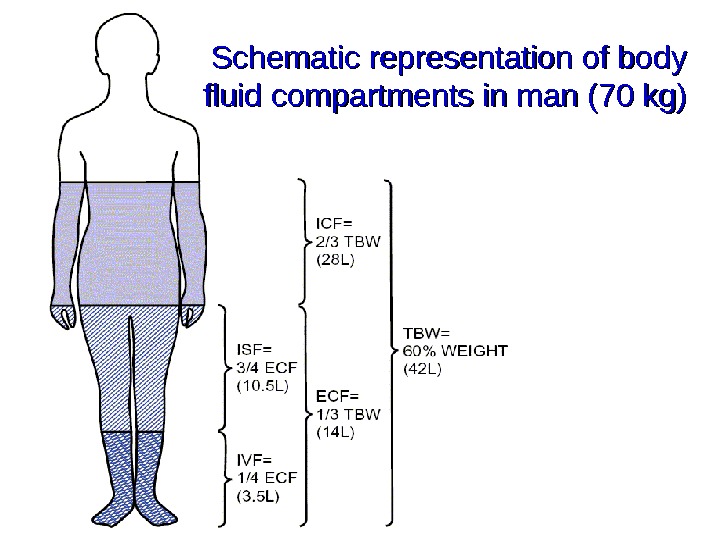
 Basics of Body Fluids • Water is primary body fluid. 40%-60% of weight in adult. Affected by age, sex, & body fat. • Distribution: 2 major compartments-ICF & ECF. • ICF: in cells. 2/3 of body fluid in adults. • ECF: outside cells. 1/3 of body fluid. 4 compartments-intravascular, interstitial, lymph, & transcellular
Basics of Body Fluids • Water is primary body fluid. 40%-60% of weight in adult. Affected by age, sex, & body fat. • Distribution: 2 major compartments-ICF & ECF. • ICF: in cells. 2/3 of body fluid in adults. • ECF: outside cells. 1/3 of body fluid. 4 compartments-intravascular, interstitial, lymph, & transcellular
 Schematic representation of body fluid compartments in man (70 kg)
Schematic representation of body fluid compartments in man (70 kg)
 Basics of Body Fluids • Intravascular: plasma • Interstitial: surrounds the cells; 3/4 ECF • Transcellular: CSF, pericardial, pleural, etc • Lymph: lymphatic system
Basics of Body Fluids • Intravascular: plasma • Interstitial: surrounds the cells; 3/4 ECF • Transcellular: CSF, pericardial, pleural, etc • Lymph: lymphatic system
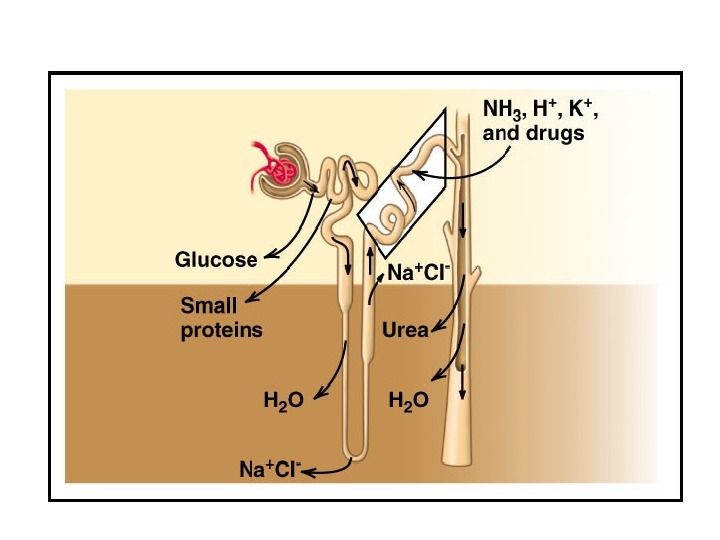
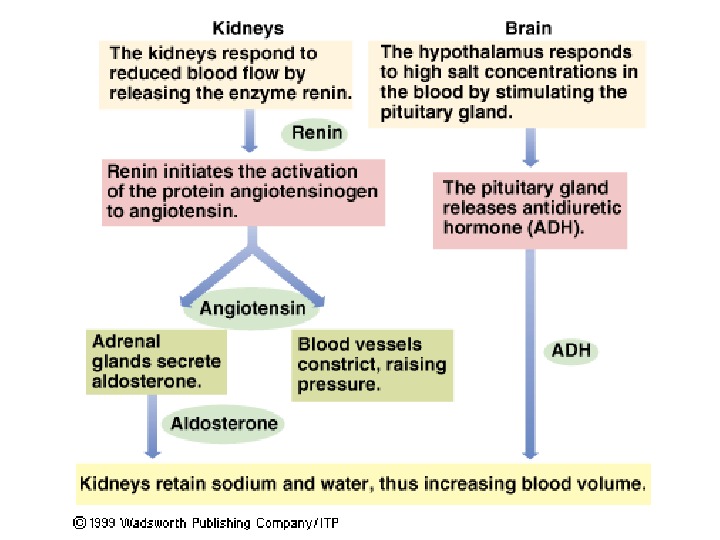
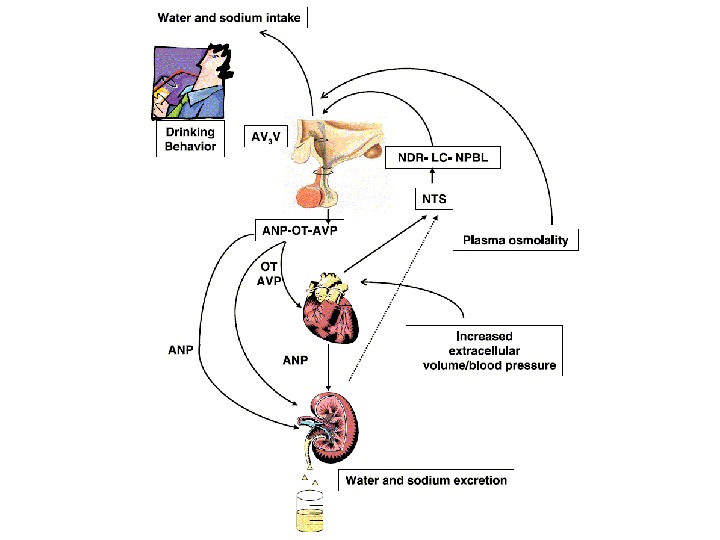
 Water Balance
Water Balance










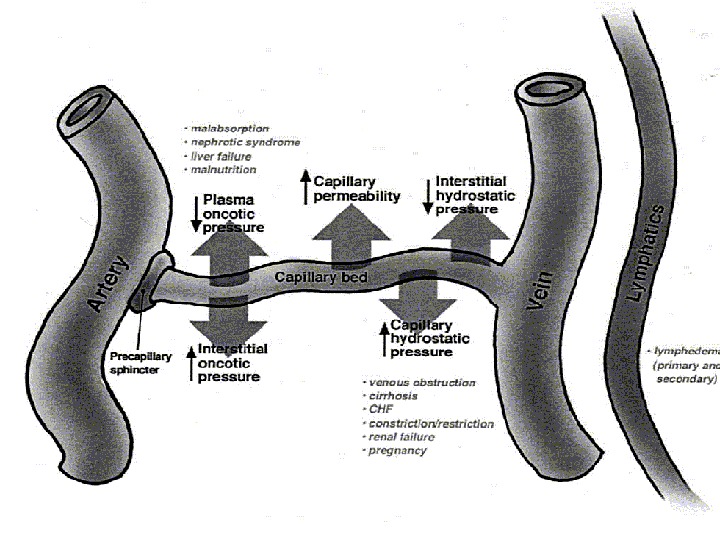
 Edema – pathological accumulation of the fluid within the extravascular space, i. e. , interstitium and/or cells Main mechanisms of edema: 1. Increased microvascular permeability (hypersensitivity type I); 2. Decreased lymph drainage (elephant leg); 3. Increased hydrostatic pressure in the capillaries (venous congestion); 4. Decreased oncotic pressure of the blood (hypoproteinemia); 5. Severe retention of water and salts (renal failure)
Edema – pathological accumulation of the fluid within the extravascular space, i. e. , interstitium and/or cells Main mechanisms of edema: 1. Increased microvascular permeability (hypersensitivity type I); 2. Decreased lymph drainage (elephant leg); 3. Increased hydrostatic pressure in the capillaries (venous congestion); 4. Decreased oncotic pressure of the blood (hypoproteinemia); 5. Severe retention of water and salts (renal failure)


